Birth Control & Contraception Options
There are several types of birth control, but at Rosemark, we want to help you find the best contraception for you.
To that end, it takes a little education on your part and we need to understand your physical makeup and emotional mind-set to best help you choose the right birth control method for you.
The following information will provide you with the insight that will help us determine, together, what birth control method will be best for you.

Birth Control Basics
While there are many forms of birth control, they all fall under two basic categories:
- Hormonal
- Non-hormonal
Both hormonal and non-hormonal birth control methods prevent pregnancy in two ways. First, by preventing the eggs from leaving the ovaries and second, by creating a barrier thus keeping sperm and eggs apart.
Play the following video for an overview of birth control options.
Types of Birth Control Methods
The following list includes options for both hormonal and non-hormonal types of birth control. They include:
- Fertility Awareness
- Barrier Methods
- Short-Term Options
- Long-Acting Reversible Contraception (LARC)
- Permanent Options
Play the following video for an overview of birth control options.
Fertility Awareness
Often referred to as the Rhythm Method or Natural Family Planning method, this type of birth control takes a lot of self-control and understanding about your own ovulation. Simply put, you track when you are ovulating. Ovulation is the period of time when you are most likely to conceive (get pregnant). During ovulation, you either refrain from sex altogether or use a barrier method of birth control during sex to prevent pregnancy.
Barrier Birth Control Methods
Barrier birth control methods include male and female condoms
| Male Condom | Female Condom |
|---|---|
A male condom is a thin sheath that is placed on the erect penis prior to and during sexual intercourse. The condom captures the ejaculate blocking the passage of the sperm.
| A female condom is a thin rubber pouch that is inserted into the vagina prior to sexual intercourse. The female condom blocks and captures the sperm ejaculated during sexual intercourse.
|
The male condom is one of the most common barrier birth control methods used today. Either male or female condoms may also be used along with spermicide-treated foam for additional protection against pregnancy.
Short Term Birth Control Options
The three most common short term birth control options include a vaginal ring, transdermal skin patch and birth control pills.
| Vaginal Ring | Transdermal Skin Patch | Birth Control Pills |
|---|---|---|
| A small flexible ring that you insert into your vagina. | This is a small adhesive skin patch you place on your skin. | These are small tablets that are taken orally once a day. |
Vaginal Ring
The vaginal ring is a flexible, plastic ring that is placed in the upper vagina. It releases estrogen and progestin that are absorbed through the vaginal tissues into the body.
The vaginal ring is folded and then inserted into the vagina. It stays there for 21 days and is then removed for a 7 day waiting period before a new ring is inserted. During the week the ring is not used, your period begins.
A healthcare provider may prescribe the vaginal ring as a continuous-dose form of birth control where a new ring is inserted every 21 days with no ring-free week in between.
Transdermal Skin Patch
The contraceptive skin patch is a small (1.75 square inch) adhesive patch that is worn on the skin to prevent pregnancy. The patch releases estrogen and progestin, which are absorbed through the skin into the body.
The patch can be placed on the chest, (except the breasts), upper back or arm, or abdomen. The patch is worn for a week at a time and a new one is put on each week for a total of 3 weeks in a row. During the fourth week, a patch is not worn, as the period commences. After week 4, a new patch is applied and the cycle is repeated.
The patch is applied on the same day of the week even if bleeding has not stopped. If continuous-dose form of this birth control is provided, a new patch is applied every week on the same day without skipping a week.

Birth Control Pills
Birth control pills are available by prescription only. There are different types of combined hormonal pills.
21-day pills: Take one pill at the same time each day for 21 days. Wait 7 days before starting a new pack. During the week you are not taking the pill, you will have your period.
28-day pills: Take one pill at the same time each day for 28 days. Depending on the brand, the first 21 pills or the first 24 pills contain estrogen and progestin. The remaining pills may be estrogen-only pills or pills that contain a dietary supplement, such as iron, but no hormones. The remaining pills may also be inactive pills that contain no hormones or supplements). During the days you are taking the hormone-free pills, you will have your period.
90-day pills: Take one pill at the same time each day for 84 days. Depending on the brand, the last seven pills either contain no hormones or contain estrogen only. With both brands, you will have your period on the last 7 days every 3 months.
365-day pills: Take one pill at the same time each day for a year. In time, bleeding may become lighter and may even stop.
Patients may expect breakthrough bleeding for approximately 3 months while their body adjusts to a change in hormone levels. It may last longer than a few months with continuous-dose pills.
Long-Acting Reversible Contraception (LARC)
Long-acting reversible contraception (LARC) is a type of birth control that lasts for an extended period of time but is not permanent.
Arm Implant
Am arm implant is a birth control method that is a progestin only contraceptive and is about the size of a matchstick. It is a long-acting reversible birth control that continually releases a low dose of progestin over a 3 year period. It is inserted under the skin of the upper arm by a specially trained Rosemark healthcare provider.
A local anesthetic will be used prior to the implant and the whole insertion only takes a few minutes.
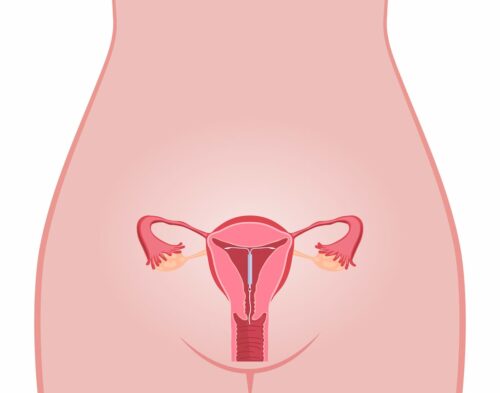
Intrauterine Devices (IUD)
An intrauterine device (IUD) is also a form of long-acting, reversible contraception.
An IUD is a small, often T-shaped device, that your doctor inserts into your uterus through the opening of your cervix.
There are two types of IUDs, copper and hormonal. See the chart below to compare the two types of IUDs as you consider one of these as your choice of birth control.
| Copper IUD | Hormonal IUD |
|---|---|
| Failure rates are about 0.8%. | Failure rate of 0.2% in the first year. |
| May stop or reduce menstruation. | May increase menstrual bleeding and result in more painful cramps. |
| Are good for up to 10 years. | Will last from 3 or 5 years (depending on the type). |
| Copper is toxic to sperm which makes the uterus and fallopian tubes produce fluid that kills sperm. | Prevents fertilization by damaging or killing sperm and making the mucus in the cervix thick and sticky so sperm cannot get through to the uterus. The uterus lining remains thin hindering egg implantation. |
Contraception Shot
This is an injection containing the hormone progestin that is given once every three months to prevent pregnancy. The hormone injection prevents your ovaries from releasing the egg into the fallopian tube.
The shot causes thick and sticky mucus in the cervix preventing fertilization and keeps the uterus lining thin, thus hindering egg implantation.
Permanent Options
Sterilization
For women who are 100% certain that they do not want to have children or do not want to have additional children, may consider sterilization as a permanent method of birth control.
| Female Sterilization | Male Sterilization |
|---|---|
| Sterilization for women is the process of closing the fallopian tubes. | Sterilization for men is the process of blocking the supply of sperm from semen. |
Female Sterilization
The procedure is commonly referred to as having one’s “tubes tied” and professionally referred to as a tubal occlusion. When the fallopian tubes are closed, the egg cannot move from the ovary to the uterus. When the sperm cannot reach the egg for fertilization, the ability to have children is removed.
For more information about permanent birth control for women, visit our Permanent Sterilization page.
Male Sterilization
This procedure, commonly referred to as a vasectomy, blocks the movement of sperm from the testicles through the small tube, called the Vas deferens. During the vasectomy, the Vas deferens is cut and sealed thus blocking the release of sperm.
At Rosemark, we do not perform vasectomies, please contact an urologist if you are interested in that procedure. For more information about permanent birth control for men, visit our Permanent Sterilization page.
Choosing The Right Method For You
The following charts will provide some insight into the various types of birth control that will help you decide with your healthcare provider, which option would be best for you.
Birth Control Effectiveness
| Most Effective | Very Effective | Less Effective |
|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Possible Side Effects
While each individual will react differently do the different birth control options, the following chart includes some of the possible side effects to non-permanent birth control. See our Permanent Sterilization page for the respective risks and cautions for those methods.
| Option | Acne | Headache | Nausea | Breast Tenderness | Vaginal Discharge | Vaginal Irritation | Weight Gain | Other |
|---|---|---|---|---|---|---|---|---|
| Male Condom | X | |||||||
| Female Condom | X | |||||||
| Other Barrier Methods | X | |||||||
| Shot | X | X | X | X | Nervousness Depression | |||
| Vaginal Ring | X | X | X | X | X | X | ||
| Pills | X | X | X | X | ||||
| Patch | X | X | X | Skin Irritation | ||||
| IUD | X | X | X | X | *See Below |
* With an IUD insertion, serious problems are rare but should be reported to a Rosemark healthcare provider right away. Complications during insertion may include:
- Bruising
- Local irritation or pain
- Itching
- Tingling, pricking or numbness
- Burning
- Bleeding
- Scarring
- Infection
A Few Notes

Here are a few notes to consider when deciding about birth control:
- Birth control options may vary while a mother is breastfeeding.
- If you are on antibiotics, you will need to use a back-up contraceptive method. Rosemark patients should make sure to tell their provider about any medicines they are taking or plan to use.
- Certain medications may make some birth control methods less effective.
- If you don’t use birth control, there is an 85% chance you will become pregnant within a year.
- Each year, 45% of all U.S. pregnancies are unplanned.
Birth Control Checklist
As you discuss birth control options with your healthcare provider,
use the following checklist to help narrow the options to find the one
best suited for your health and lifestyle.
Main Reasons for Seeking Birth Control
- I only want to use birth control to prevent pregnancy.
- I want to use birth control but for other reasons, like to prevent acne.
Plans for children
- I’m definitely, 100% positive, that I never want to have children.
- I want children, but not within the next 5 – 10 years.
- I want to have children fairly soon, but just not now.
Feelings about your Period on Birth Control
- I don’t really want to have a period at all.
- I feel more at ease having a regular period.
- It would like to have consistent, regular periods.
Daily Habits
- I have no problems remembering to take my medicine on a daily basis.
- I’m not reliable when it comes to remembering daily tasks, like taking daily medicine.
- I eat fairly well and get good exercise.
- I smoke.
Thoughts about Birth Control
- I don’t think I would have the self-control to insert birth control before sex.
- I like the idea of a long-term birth control methods so I don’t have to constantly worry about it.
- I don’t mind a trip to the doctor’s office every few months to get birth control.