Uterine Fibroids

Uterine fibroids, also called uterine myomas, leiomyoma, leiomyomata and fibromyoma, are benign non-cancerous growths that develop from the muscle tissue of the uterus.
Uterine fibroids may be present inside the uterus, on its outer surface or within its wall. They may also be attached to the uterus by a stem-like structure.
The size, shape, and location of uterine fibroids can vary greatly. While some women may only have one fibroid other may have many of varying sizes.
A fibroid may remain very small for a long time and suddenly grow rapidly, or it may grow slowly over a number of years.
WHO IS AT RISK
Fibroids are most common in women 30 – 40 years of age but they can occur at any age. Between 20 – 50% of women of childbearing age have uterine fibroids. Fibroids occur more often in African American women than in white women. They also seem to occur at a younger age and grow more quickly in African American women.
COMMON SYMPTOMS
Common symptoms of uterine fibroids include:
- Very Heavy & Prolonged Periods
- Severe Menstrual Cramps
- Pain in the Back of the Legs
- Pelvic Pain or Pressure
- Pain During Intercourse
- Bladder Pressure, Difficult & Frequent Urination
- Bowel Pressure & Constipation
- Rectal Pain & Difficult Bowel Movements
- Enlarged Abdomen & Uterus
- Recurrent Miscarriages or Infertility Problems
While these symptoms are common, there are women who have fibroids but have no symptoms at all.
TYPES OF UTERINE FIBROIDS
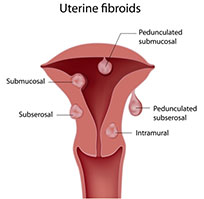 There are four different types of uterine fibroids:
There are four different types of uterine fibroids:
- Sub serosal Uterine Fibroids develop in the outer portion of the uterus and continue to grow outward.
- Intramural Uterine Fibroids are the most common type of fibroid. They develop within the uterine wall and expand making the uterus feel larger than normal.
- Submucosal Uterine Fibroids develop under the lining of the uterine cavity. These fibroids have the most effect on heavy menstrual bleeding and the ones that can cause problems with infertility and miscarriage.
- Pedunculated Uterine Fibroids grow on a small stalk that connects them to the inner or outer wall of the uterus.
Uterine fibroids are rarely associated with cancer.
DIAGNOSIS

Ultrasound, hysteroscopy, and laparoscopy are the typical methods that health care providers use to diagnose uterine fibroids.
Imaging tests, such as magnetic resonance imaging and computed tomography scans, may be used but are rarely needed. Some of these tests may be used to track the growth of fibroids over time.
Women and their Rosemark health care provider will discuss and decide on the appropriate treatment for uterine fibroids based on individual circumstances. Certain signs and symptoms warrant treatment such as:
- Heavy or painful menstrual periods that cause anemia.
- Heavy or painful menstrual periods that disrupt a woman’s normal activities.
- Bleeding between periods.
- Uncertainty of the nature of the growth.
- A rapid increase in growth infertility, miscarriages or pelvic pain.
TREATMENT
There are a few treatment options for uterine fibroids.
DRUG THERAPY
Drug therapy is an option for some women with fibroids. Medications may reduce the heavy bleeding and painful periods that fibroids sometimes cause. They may not prevent the growth of fibroids. Surgery is often needed later.
SURGERY
Myomectomy is the surgical removal of fibroids while leaving the uterus in place. Because a woman keeps her uterus, she may still be able to have children. Fibroids do not regrow after surgery, but new fibroids may develop. If they do, more surgery may be needed.
Hysteroscopy is used to remove fibroids that protrude into the cavity of the uterus. A resectoscope is inserted through the hysteroscope. The resectoscope destroys fibroids with electricity or a laser beam. Although it cannot remove fibroids deep in the walls of the uterus, it often can control the bleeding these fibroids cause.
Hysterectomy is used to remove the uterus. The ovaries may or may not be removed during a hysterectomy. A hysterectomy is a last resort and is done when other treatments have not worked or are not possible or the fibroids.
SUMMARY
If you are experiencing symptoms of uterine fibroids, please give us a call and your Rosemark board certified gynecologist will help you get feeling better.